Early Online (Volume - 9 | Issue - 1)
Cystoid Macular Oedema Secondary to Bimatoprost in a Patient with Primary Open Angle Glaucoma
Published on: 7th April, 2025
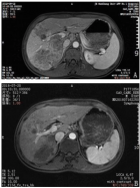
Cystoid Macular Oedema (CMO) is a condition characterized by fluid accumulation in the macular region of the retina, leading to the formation of cyst-like spaces. This edema often results in visual impairment and is associated with various ocular and systemic conditions, including surgery, inflammation, or medication use. The authors present a case where Cystoid Macular Oedema (CMO) occurred after commencing topical bimatoprost in a pseudophakic patient with primary open angle glaucoma. The macular oedema was treated effectively with a combination of non-steroidal and steroidal topical drops. This case report shows a possible correlation between bimatoprost and CMO, in a patient with no recent confounding risk factors known to contribute to CMO . The recommendation from this report is that all patients treated with topical bimatoprost drops should have a baseline macula OCT examination and a repeated OCT examination 8 weeks after initiation of treatment, to facilitate early detection of CMO.
Comparison of Visual Field Progression in Patients with Primary Open Angle Glaucoma and Pseudo Exfoliative Glaucoma
Published on: 9th May, 2025
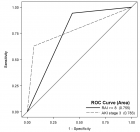
Objective: Comparison of visual field progression in patients with Primary Open-angle Glaucoma (POAG) and Pseudo Exfoliative Glaucoma (PEXG).Methods and materials: This is a 2-year longitudinal prospective study including 60 glaucomatous eyes with VA CF ≥ 3 m, IOP ≥ 20 mmHg, CDR ≥ 0.6 and those with Shaffer’s grade 3 or above were categorized as POAG along with signs of Pseudo exfoliative material as PEXG.Patients on anti-glaucoma medications and those who have undergone cataract and glaucoma surgeries are also included in this study. 24-2 visual field test was performed using Humphrey Field Analyzer & the progression was assessed based on 3 parameters- Mean Deviation (MD), Visual Field Index (VFI) & Guided Progression Analysis (GPA).Results: The difference in MD & VFI was higher in PEXG (-5.77 dB) (10.88%) than in POAG (-1.56 dB) (7.17%) respectively & was significant statistically (t - test, p = < 0.001). The GPA showed fast progression in 53.30% of cases in PEXG, 13.30% in POAG (Chi-square, p = < 0.001) about 63.30% of POAG & 46.70% of PEXG showed slow- moderate progression, but 23.30% of POAG subjects had no progression.Conclusion: Compared to POAG, the study showed that PEXG had frequent & faster visual field worsening. Therefore, PEXG patients require more stringent management & treatment than those with POAG.
Impact of Refractive Error Correction on Vision Related Quality of Life in School-Aged Children-A Prospective Interventional Study
Published on: 23rd May, 2025
Aim: To compare the vision related quality of life before and after prescription of refractive glasses in school-aged children. Design: A prospective, comparative, and hospital-based interventional study was conducted at the Regional Institute of Ophthalmology, PGIMS, Rohtak between May 2021-May 2022. It involved assessment of vision-related quality of life (VRQoL) in 200 school-going children of the 5-16 age group, then comparing outcomes in children with URE versus those corrected with eyeglasses. Those with significantly low visual acuity (≤ 6/9) on Snellen’s were enrolled in the study after obtaining written informed consent from parents. The Modified SREEQ was used to assess VRQoL. Various parameters of comparison included age, gender, demography, education, and improvement in VRQoL within individual study groups over time. Comparison was done before and after using prescription refractive eyeglasses with a follow-up period of 3 months. Results: The correction amongst hypermetropes, 40 out of total 200 students (20%), correction among myopes (153 of 200 students), correction amongst students with astigmatism (7 out of 200 students) resulted in changing categories from mild/moderate/severe visual impairment to normal category of visual acuity i.e., 6/6 on immediate correction with refractive glasses prescribed to them post refraction. Students with astigmatism showed an improvement in symptoms like distorted images post-refractive correction at 3 months. Thus, proving a positive role of refractive eyeglasses in reducing the burden of refractive errors in our study population and improving the visual outcome. Conclusion: VRQoL was better in students after they got their refractive errors corrected with prescription eyeglasses at 3 months as compared to their QoL evaluated at their first visit to our centre with URE. This study focused on having a holistic approach towards improvement in QoL by taking into consideration the academic, psychological, cost-effectiveness aspects of VRQoL among students in the age group 5-16 years old.
Custard Apple Seed Induced Bilateral Toxic Keratoconjunctivitis - A Case Report
Published on: 23rd June, 2025
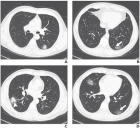
Custard apple is a tropical fruit that is cultivated all over India. The seeds of this fruit are found to have medicinal properties as they contain active compounds such as alkaloids, cyclohexapeptides, and acetogenins. It has been used in powdered form for the treatment of scalp lice and dandruff in our part of the world as a native medicine for a long time. We report a case of bilateral severe toxic keratoconjunctivitis following accidental exposure to custard apple seed powder.

HSPI: We're glad you're here. Please click "create a new Query" if you are a new visitor to our website and need further information from us.
If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."